Nov 14
2022
RCM and Coding May Help Close Health Equity Gap

By Leigh Poland, RHIA, CCS, AGS Health.
Health equity is a focus of providers, regulatory agencies, and payers as they seek ways to eliminate care disparities across race and ethnicity, gender, sexual orientation, and socioeconomic status lines. Its significance is further impacted by new quality-based care models beyond those established by the Patient Protection and Affordable Care Act of 2010.
The challenge for many healthcare organizations participating in these new reimbursement models is how to view health equity and social determinants of health (SDoH) to understand the actual value of this information. Often overlooked is that healthcare organizations’ coding and revenue cycle management (RCM) departments already aggregate information that can help better understand inequities in care delivery and health equity across their patient populations.
A Primer on SDOH Impacts
SDoH impact many health risks and outcomes, which is why this data is vital for clinical care and reimbursements. Defining factors can include anything from geography, race, gender, and age to disability, health plan, or any other shared characteristic. Of increased importance, SDoH issues are most often experienced by the most vulnerable members of society: the poor, less educated, and other disadvantaged groups.
SDoH is linked negatively with outcomes, including higher hospital readmissions, length of stay (LOS), and increased need for post-acute care. Value-based payment programs, therefore, may penalize organizations that disproportionately serve disadvantaged populations if they do not collect and respond to SDoH data.
For example, addressing food insecurity — a key SDoH data point — by connecting patients to programs like Meals on Wheels, Supplemental Nutrition Assistance Programs (SNAP), or food pantries is proven to reduce malnutrition rates and improve short and long-term health outcomes.
In the case of SNAP, which is the primary source of nutrition assistance for more than 42 million low-income Americans, participants are more likely to report excellent or very good health than low-income non-participants. Low-income adults participating in SNAP incur about 25% less medical care costs (~$1,400) per year than low-income non-participants.
RCM and Health Equity
Between the financial impact of addressing SDoH and new reimbursement models that emphasize health equity, there is a strong business case for involving RCM in any comprehensive health equity/SDoH strategy. Why? Because health disparities contribute $93 billion in excess medical care costs and $42 billion in lost productivity per year. If these inequities were eliminated by 2050, it would reduce the need for more than $150 billion in medical care.
Reimbursement is closely linked to quality, which SDoH affects because of the use of outcome measures by the Centers for Medicare & Medicaid Services (CMS) to determine a hospital’s overall quality, including mortality, the safety of care, readmission rate, excess stay, patient experience, and effectiveness of care.
Readmission rates, utilization, and excess inpatient stays, in particular, tie back to SDoH:
- Low literacy is linked to poor health outcomes and less frequent prevention services, meaning more frequent and longer hospital stays.
- Lack of access to reliable transportation for basic health needs results in 41% more excess days in the hospital.
- Unemployment is linked to declining self-reported health status, increased mortality rates for those ages 16 through 64, quadruple rates of drug and substance abuse and dependence, and double the chances of being diagnosed with a mental disorder.
Coding and RCM professionals interact daily with information that is valuable to health equity strategies, notably since the transition to ICD-10 created an environment rich with data detailing SDoH. Including this documentation within the patient’s medical record helps address SDoH and narrow health equity gaps.
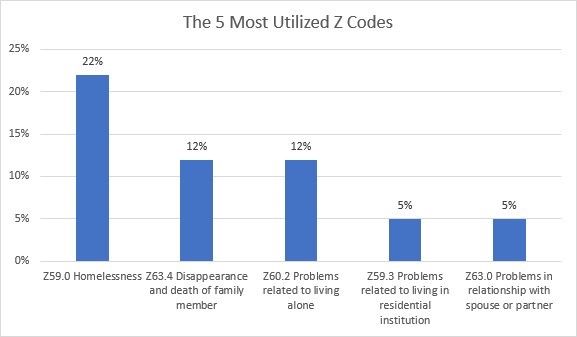
Source: CMS Office of Minority Health. “Utilization of Z Codes for Social Determinants of Health among Medicare Fee-for-Service Beneficiaries, 2019”. Data Highlight NO. 24 | September 2021. Nov. 7, 2022. https://www.cms.gov/files/document/z-codes-data-highlight.pdf
Additionally, establishing a governance committee can help sort collected data and design policies and procedures to ensure SDoH needs are assessed and patients are linked to the community services needed to address them.
However, of the 56% of organizations reporting in an AHIMA survey that they collected SDoH data, 73% said they had yet to establish a governance committee. Oversite allows for determining who is tasked with conducting patient assessments and how best to gather data without creating an administrative burden.
In addition to establishing a governance committee, healthcare organizations need to address four data concepts to integrate SDoH with clinical data and care plans fully:
- Screening tools: Numerous existing tools can be leveraged to identify patients with social risk factors, including some embedded within electronic health record systems.
- Diagnosis/Identified need(s): Reporting SDoH issues identified by screening tools.
- Interventions: Actions taken to address the specific SDoH needs.
- Goals: Results expected to be achieved to resolve the patient’s identified need(s).
It is also important to conduct audits on documentation quality and coding accuracy and provide appropriate feedback.
SDoH For Improved Care
Health equity is expected to remain a top priority for the near term, as evidenced by CMS recently releasing its Framework for Health Equity and proposed rules to advance health equity.
Healthcare providers are increasingly becoming community stewards of this initiative. To begin addressing more than basic catch-and-patch care, health systems must explore opportunities to eliminate disparities and improve care among underserved communities.
The data aggregated daily by coding and RCM departments can be pivotal for identifying and understanding population needs and aligning patients with the resources to address SDoH issues and close the health equity gap.